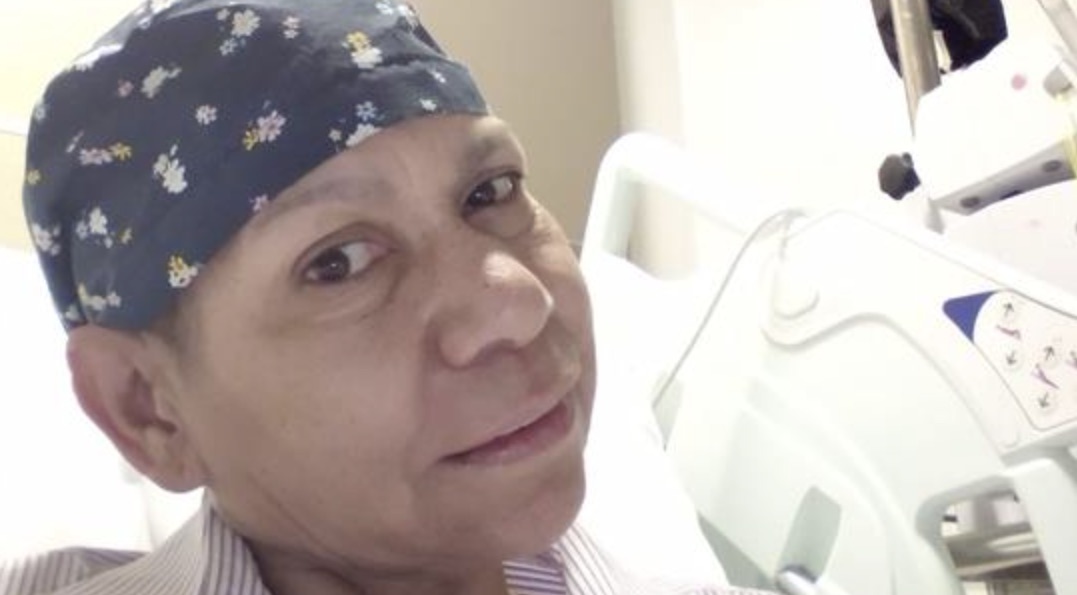
First Nations Australians dying at far higher rates from blood cancer
Blood cancer is one of Australia’s most rapidly rising cancers yet new research shows First Nations Australians fare much worse than most – revealing a dire situation and a national public health and equity issue.
First Nations people diagnosed with blood cancer are up to five times more likely to die from the disease, than non-Indigenous Australians.
And the five-year survival rate for Indigenous Australians diagnosed with blood cancer is 11 per cent lower than non-Indigenous Australians.
New research shows they are dying at a much younger age, face major barriers contributing to the survival gap, and systemic inequities which place more lives at higher risk.
Better awareness
Lynette Liddle and Jackie Henderson are two survivors who are calling for better awareness of the disease in First Nations communities as well as for better understanding of cultural needs within the many health services that operate on country, State and nationwide.
Lynette, from Alice Springs, was diagnosed three years ago when internal bleeding saw her flown by the Royal Flying Doctor Service to Adelaide, where surgery discovered the issue.
“It was really by chance,” Lynette told First Nations News.
“And I didn’t know what it was. What have I got, what happens next?”
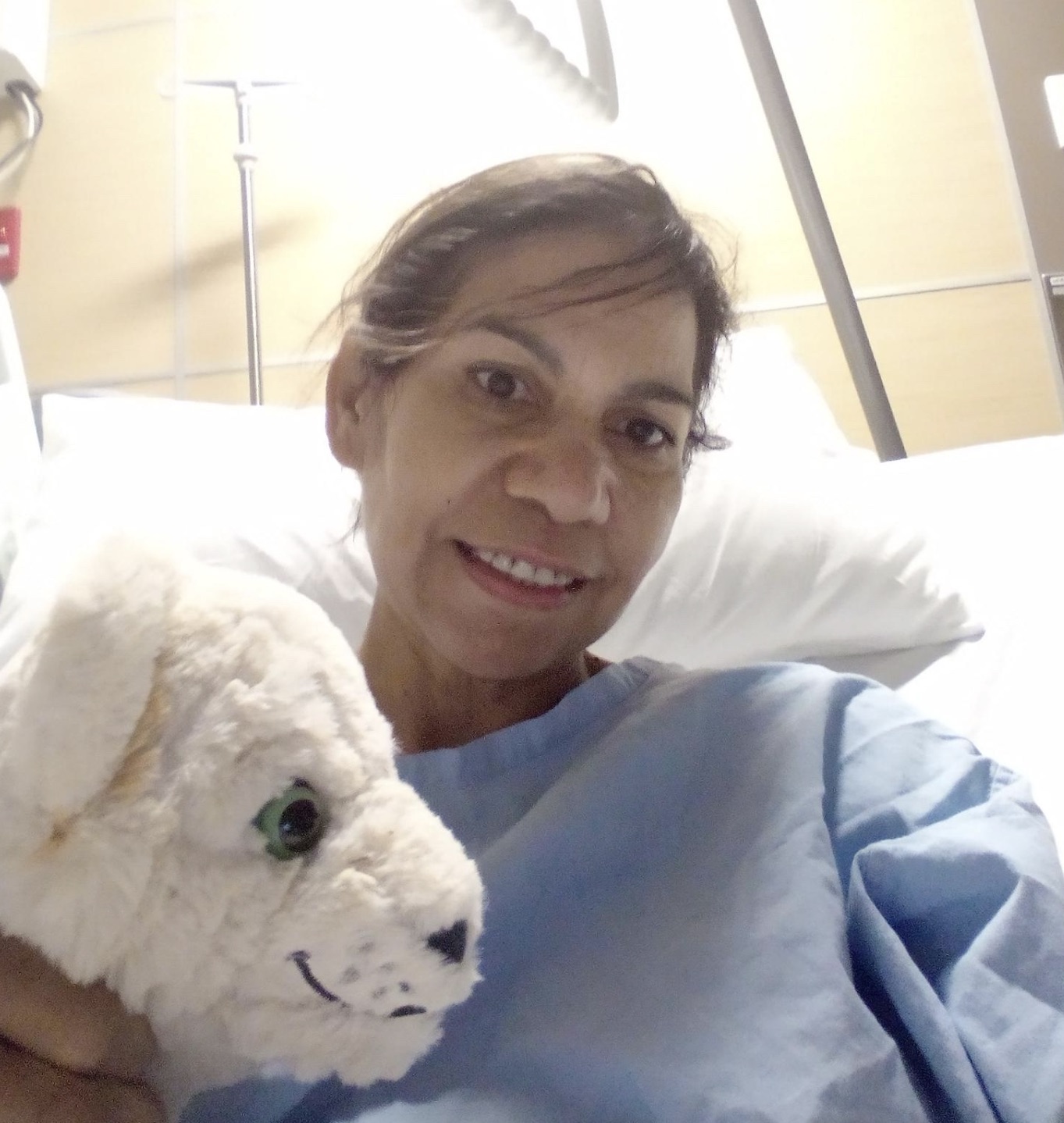
Lynette Liddle said her diagnosis was by chance.
Major barriers found contributing to the survival gap in First Nations Australians v’s non-Indigenous Australians include:
- Low awareness and late diagnosis: Awareness of blood cancer symptoms is low leading to increased delayed diagnosis and impacting survival outcomes.
- Treatment access slowed by distance and cost: Most First Nations blood cancer patients live in regional / rural Australia – travelling hundreds or thousands of kms for specialist care – leading to delayed diagnosis, interrupted treatment, and intense financial stress. Carers face major emotional, practical and economic burdens with little formal support.
- Lack of culturally safe information and care: Patients receive information that is unclear, non-tailored or culturally inappropriate, including inconsistent instructions and limited engagement with Aboriginal Liaison Officers due to patchy availability.
- Workforce gaps in cultural capability: Health professionals are under-resourced and under-prepared to meet the cultural, social and informational needs of First Nations patients, despite a strong desire to improve.

Lynette, who is now in remission says more Aboriginal nurses are needed.
Lynette is a single woman and she struggled to cope. How would she pay her mortgage. With no family support, who would assist with the out of pocket expenses?
“I had no income support and there wasn’t much cultural support either – which has to change,” Lynette, who now lives in Adelaide, said.
“Rural health has its problems and needs more staff, more Aboriginal nurses who understand.
“My mum was a nurse and experienced so much racism back then, but we are all human beings and it’s important to have respect for each other.
“It comes down to trust and Aboriginal people need others around them they can trust and know. It’s so important. Partnership and in pairs. Don’t be alone.”

Lynette is now in remission, although she prefers to say, ‘Yep, I’m fine”.
Her prognosis is good, but she still has medication to take and she needs to get regular tests.
“My advice to anyone with a health problem is to speak to a doctor and get tested, early. And don’t be afraid of leaving country if you have to.
“It would be great to have more facilities on country and I would love to see an Aboriginal hospital that understands our needs, but we need to trust the doctors treating us.”

Lynette says she would love to see an Aboriginal hospital that ‘understands our needs’.
Australia’s healthcare system, says the Leukaemia Foundation, is not working for First Nations Australians. They face major inequities at every step of the cancer journey – from diagnosis to survivorship.
While Australia is improving outcomes for non-Indigenous Australians, sadly Indigenous people still lag far behind.
Grandmother Jackie Henderson, from Port Stephens in NSW, discovered she had blood cancer in 2020.
“Dry eyes and mouth, fatigue, big weight loss. I dropped from 78kg to 53kg quickly. Once I saw a specialist, and after a series of checks, I was diagnosed with Angioimmunoblastic T Cell Lymphoma.

Jackie with the Leukaema Foundation’s head of research, Bill Stavreski.
“I said to my husband: ‘What’s that?”
Jackie admitted that in Mob man in the past have given up when diagnosed. But she was different.
“I was not going to lie down and die,” she said. “And I told everyone that.
“I don’t think there is enough information and awareness of cancers in our Mobs.
“It is NOT end of life – if you catch it early.”
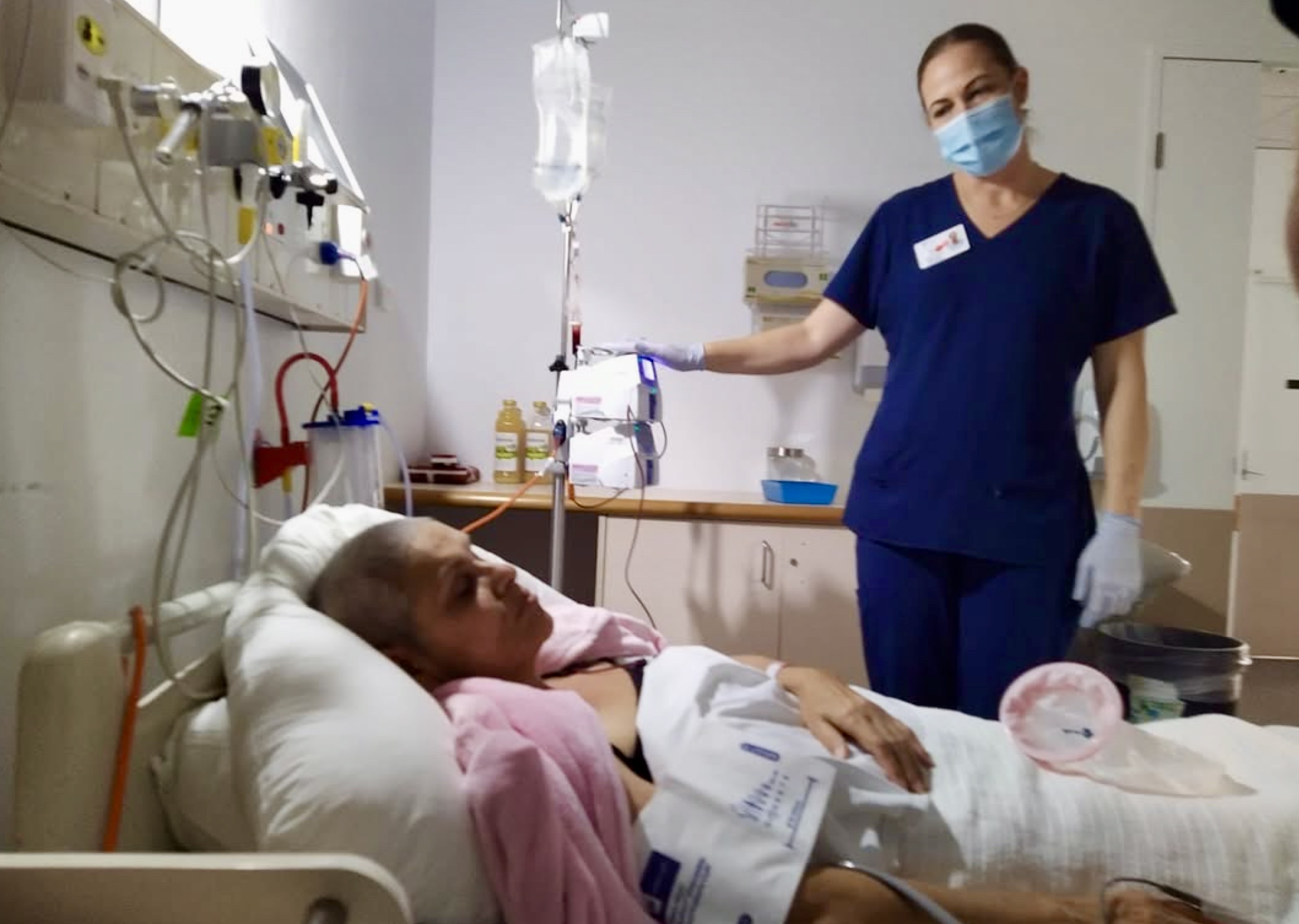
Jackie would like to see more resources to educate remote communities.
Jackie would like to see an organisation like the McGrath Foundation, that could go out to remote communities and educate people on blood cancers.
“I live on the coast, but out there they don’t have resources, they don’t have the luxury of transport to get to hospitals,” she said.
“And to those who wonder, yes, it is OK to come off country to get treatment. It is daunting and we do need more support. But it is a positive way forward.”
New research has provided a roadmap for action, with clear guidance for improving outcomes for First Nations people, beyond improving medical treatment alone, the Leukaemia Foundation says.
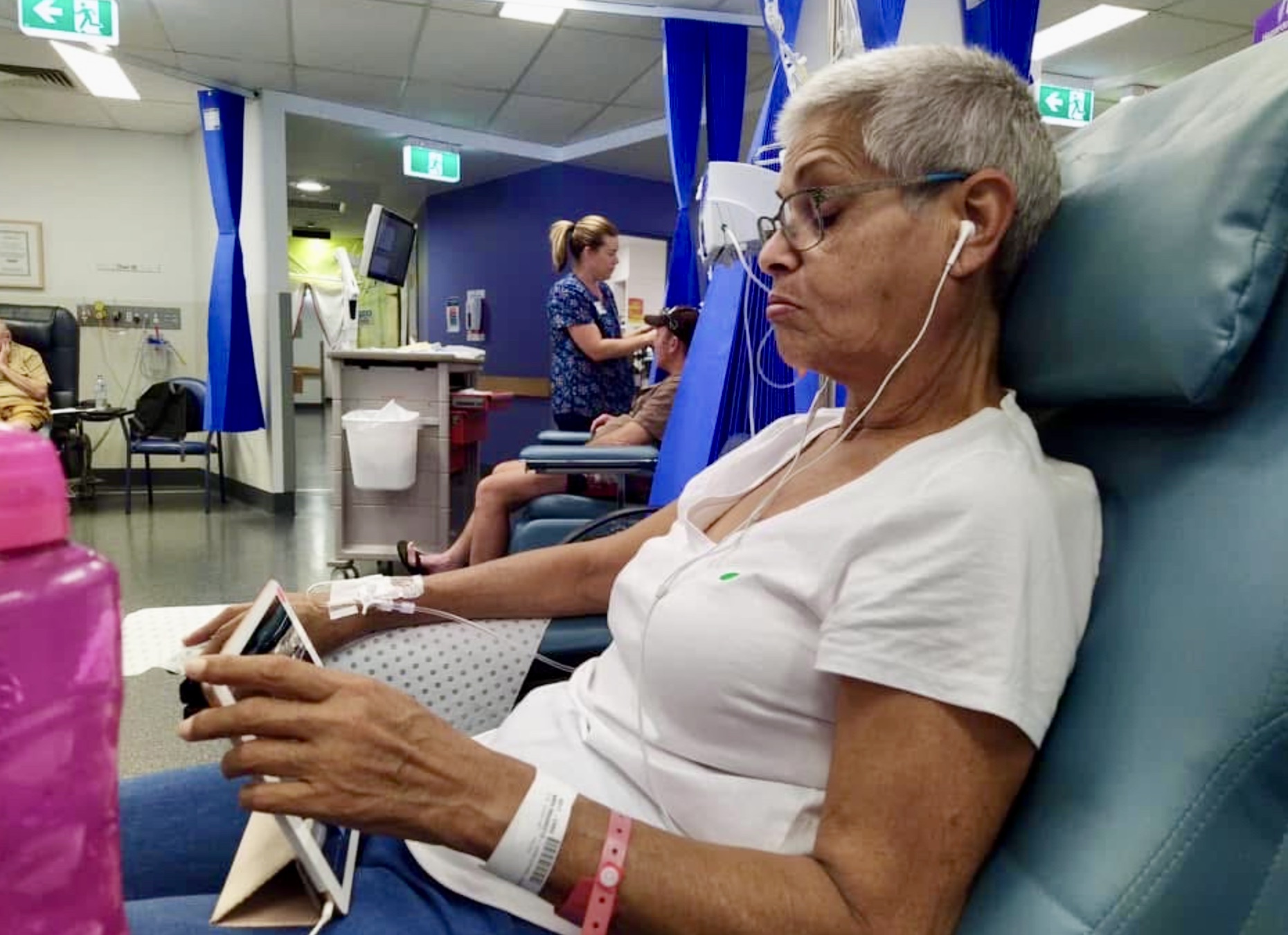
If there are changes talk to your doctor and don’t be afraid of the health system, Jackie says.
“Issues must be tackled head on to combat the delay in diagnosis including educating First Nations Australians on blood cancer and the most common signs and symptoms, AND strengthening cultural safety, improving access to information and support, and expanding culturally tailored blood cancer services.”
Jackie has had her family for support. Her husband, children and grandchildren, but she knows others in remote Australia may not have that.
“But listen to your body, If there are changes talk to your doctor and don’t be afraid of the health system.”
The Leukaemia Foundation supports many First Nations Australians and they are on a mission to reach every person affected by blood cancer and provide crucial support and services to minimise impacts and invest in vital research.

Jackie has had her family for support. Her husband, children and grandchildren.
Did you know
- Indigenous Australians diagnosed with blood cancer are twice as likely to be diagnosed under 35 years of age; and three times more likely to die from the disease under 50 years old compared to non-Indigenous Australians.
- The numbers of Indigenous children (under 15 yrs) diagnosed with blood cancer is 3 times higher than non-Indigenous children.
How all Australians can help
World Cancer Day – Wednesday February 4
With First Nations Australians diagnosed with blood cancer faring much worse than non-Indigenous Australians, the Leukaemia Foundation needs Australia’s help to raise critical funds so it can continue supporting First Nations families across the country and to further invest in groundbreaking blood cancer research.
The Leukaemia Foundation is encouraging Australians help us support First Nations people diagnosed with blood cancer by signing up to its iconic fundraising campaign, the World’s Greatest Shave, which aims to raise $12 million dollars this year. People can shave, cut, or colour their hair in support of First Nations Australians living with blood cancer.
Funds raised from the World’s Greatest Shave ensures the Leukaemia Foundation can fund crucial blood cancer research as well as assist patients and families with accommodation while they are undergoing treatment, assistance with transport to appointments, education and information around their specific type of cancer, as well as other practical, financial, emotional and mental health support.







